Parandotitis
What is it about?
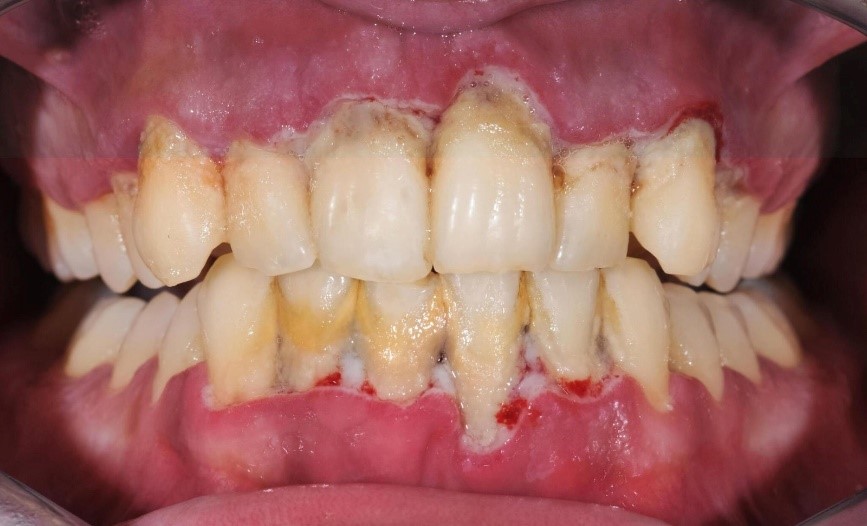
Periodontitis or periodontal disease is a chronic oral inflammatory polymicrobial disease which progressively destroys the structures of the periodontium, i.e. the tooth support apparatus (periodontum: gum and bone) , and which – if not stopped in time – can lead to the progressive loss of teeth.
In summary, it is a bacterial pathology which, due to the body’s inflammatory response, leads to the progressive resorption of the alveolar bone (i.e. the bone that keeps the teeth functioning), with retraction of the gums and serious aesthetic and of chewing. The presence of bacteria that accumulate inside the gingival sulcus produces a progressive detachment of the gum with resorption of the bone, causing the formation of a space, called periodontal pocket , which further favors the accumulation and growth of bacteria with worsening of the condition of the tissues .
Periodontitis: the symptoms
- Gingivitis: superficial inflammation of the gums which become swollen, red and bleed easily;
- Bleeding: this can occur during tooth brushing or chewing or can be spontaneous, detected in the morning due to the presence of blood stains on the pillow;
What happens to the teeth?
- they lengthen due to the retraction of the gums;
- they become unstable;
- sometimes they change their position.
Chewing also becomes difficult and sometimes painful. Repeated abscesses may appear in the areas of greatest severity, i.e. where the detachment of the gum (pockets) is deepest.
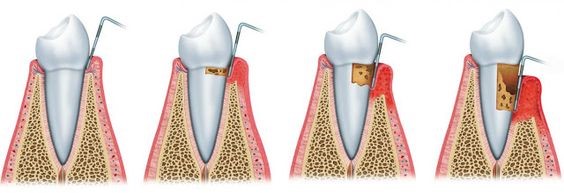
The causes of periodontitis
Periodontal disease is defined as a multifactorial disease , i.e. numerous factors participate in its appearance:
- general factors: the most frequently involved are diabetes , smoking and obesity .
- genetic factors that cause a reduced defense capacity;
- bacteria , called periodontal pathogens , which are the primary etiological agents;
Smoking: there are many studies that demonstrate the correlation between smoking and periodontal disease.
The smoke:
- the probability of incurring pyorrhea greatly increases ;
- significantly reduces the response to therapy .
Smoking, in fact, significantly limits vascularization and has a negative effect on the body’s immune defense response : the ability of cells such as polymorphonuclears to arrive from the bloodstream and act to destroy bacteria (reduction of chemotaxis, production of enzymes and phagocytosis) is profoundly limited. Furthermore, the destruction of the gum tissues is related to the duration and quantity of smoke to which the tissues have been exposed.
Diabetes
Periodontal disease also has a particular relationship with diabetes , so much so that it is defined as a two-way relationship: those who suffer from diabetes have a 3 times greater risk of getting periodontitis, and those who suffer from this pathology increase the probability of having diabetes or seeing it. get worse. In fact, the inflammatory reaction typical of periodontal disease is altered by high levels of glucose in the blood, causing a worsening of gum conditions. On the other hand, Parodotitis can influence diabetes due to the large quantities of inflammatory products and bacteria that can enter the circulating blood and reach various organs, including the pancreas, causing inflammatory reactions with worsening of its functions.
Obesity
The relationship between obesity and periodontitis is also well documented: obese or overweight subjects are more likely to have periodontitis than normal weight people. The biological motivation is mainly constituted by the fact that adipose cells produce large quantities of pro-inflammatory cytokines , which increase the inflammatory state of the subject with worsening of periodontal disease. In the same way, the increase in the inflammatory state increases insulin resistance, worsening diabetes.
Psychological causes of periodontitis
Some scientific studies have identified stress , anxiety and depression as risk factors for the onset of periodontal disease . Stress can in fact generate a series of negative physiological responses in the individual which, in short, would alter the body’s immune defenses.
How long does it take for periodontitis to appear?
Periodontitis generally manifests itself in mature age and has a slow and constant course over time, but sometimes it can also affect young adults ( aggressive or rapidly progressive form ); in this case the progression is quicker.
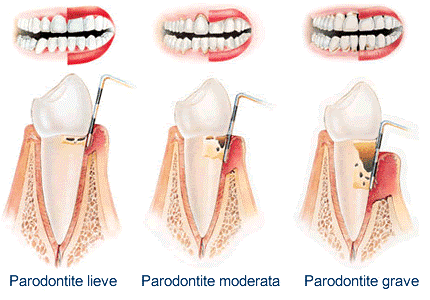
What are gum pockets?
If the inflammation of the periodontium persists and becomes chronic, the gum detaches from the tooth and the formation of so-called ” gingival pockets ” (dental pockets or gingival pockets).
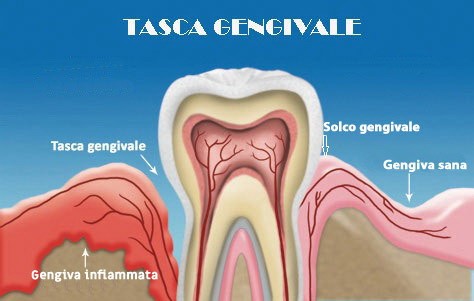
The pockets will act as a receptacle for subgingival tartar and bacteria. In the strenuous fight between bacterial toxins and immune defenses, the one who loses out is the alveolar bone, which will progressively reabsorb upwards until the tooth is left exposed. As a result, the tooth without surrounding bone will begin to loosen until it falls out , in the absence of appropriate diagnosis and treatment.
Why do teeth move?
Teeth that move together with receding gums and gum bleeding are the periodontitis symptoms that most alarm patients, immediately making them think of periodontitis. This happens because the bacteria attack and inflame the tooth support system (periodontal ligament, gum and bone). The mobile tooth can become stable again if periodontitis is diagnosed and treated in time.
In most cases, tooth mobility is attributable to periodontitis but sometimes it can also be due to an endodontic problem (tooth to be devitalized) or excessive teeth grinding which is why it is important that the diagnosis is made during the visit . by a dentist experienced in periodontitis.
Teeth moving remedies. Most of the time the treatment for moving teeth is the same as for periodontitis treatment; in other cases, however, it depends on the diagnosis made. If the origin of the mobility is an endodontic problem, root canal treatment must be performed and if the tooth that moves is due to excessive grinding, bruxism must be treated.
The consequences of periodontitis if left untreated
If untreated, periodontal disease therefore causes tooth loss and contributes to the onset of systemic diseases . Additionally, it is a significant risk factor for:
- cardiovascular diseases;
- pre-term births in pregnant women ;
- diabetes .
All these general conditions can be traced back to the presence of large quantities of pro-inflammatory molecules which are released into the bloodstream, reaching some target organs.
Correlation between heart attack and periodontitis
Is there a correlation between heart attack and periodontal disease? Unfortunately the answer is yes . Studies have highlighted a link between periodontal disease and cardiovascular disorders which is expressed through two different mechanisms. A direct mechanism that consists in the migration of periodontal pathogenic bacteria from oral tissues to other organs, via the bloodstream (bacteremia).
The indirect mechanism instead refers to the production, by the bacteria that cause periodontal disease, of inflammatory mediators capable of reaching the circulatory system and causing vascular damage even remotely. It can therefore be stated that there is a direct association between untreated periodontal disease and the increased risk of myocardial infarction and ischemic stroke .
Diabetes and periodontitis
Are diabetic patients more exposed to periodontitis? The answer is yes .
Diabetic patients, especially those who cannot keep their blood sugar under control, suffer from gingivitis and periodontitis more frequently than non-diabetic patients. Some scholars have defined periodontitis as ” the sixth complication of diabetes “. Unfortunately, the mechanism underlying this phenomenon has not been perfectly clarified. Therefore, people with diabetes must pay particular attention to their gums and undergo periodontal treatment as soon as possible if this pathology is diagnosed.
Pregnancy and post-natal complications
Various research hypothesizes a link between periodontal disease during pregnancy and the risk of premature birth, with all the consequences that may result for the newborn.
Furthermore, it must be taken into account that the hormonal variations typical of pregnancy can lead to a worsening of the health of the gums, which becomes difficult to manage if you start from a non-optimal state.
The diagnosis of periodontitis
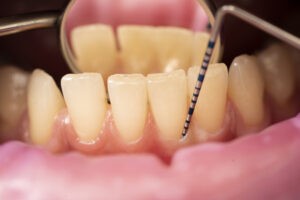
The diagnosis of periodontal disease (pyorrhoea) is made very simply and non-invasively using a millimeter instrument, the periodontal probe , which is slid between the surface of the root and the gum and allows the presence of notches to be assessed and to be measured. the severity of the injury.
Naturally, to evaluate the morphology of the bone destruction it will be necessary to follow the survey with intraoral radiographs .
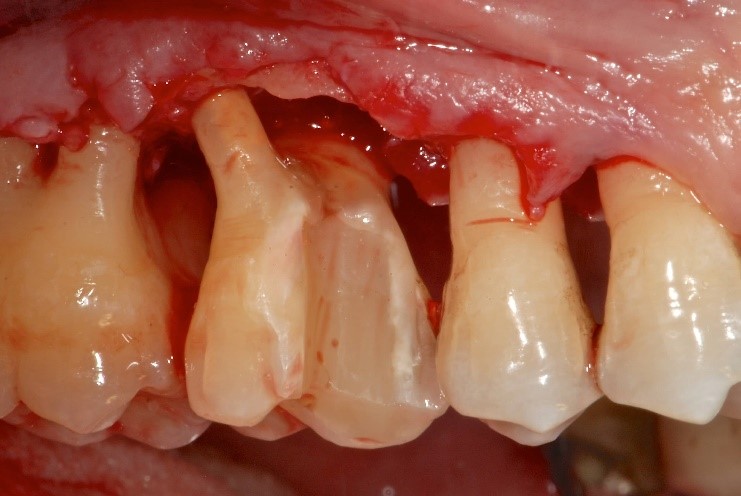
How periodontitis is treated
The first phase of therapy consists of:
- removal of bacteria (bacterial plaque) and mineral concretions (tartar) above and below the gums;
- give information on how to improve the quality of oral hygiene ;
- implement a precise fight against smoking ;
- provide correct dietary suggestions and correct lifestyles.
Following the first local therapy sessions, which as mentioned consist of oral hygiene instructions, removal of tartar above and below the gums and superficial portions of the root (cement) if infected, the patient is re-evaluated for any secondary needs. This first therapeutic phase, which may represent all that is necessary to do, is carried out by the dentist or dental hygienist
In cases where this first therapeutic phase does not correspond to the elimination of the pockets or the complete resolution of the tissue problems, in the more serious and more advanced cases the therapy becomes the responsibility of the dentist who mainly deals with periodontology. If not managed or, worse, underestimated and not treated in time, periodontal disease evolves into pyorrhea , the final phase in which tooth loss inexorably and progressively occurs, with consequent reabsorption of the alveolar bone (i.e. the bone that keeps the teeth in place). function).
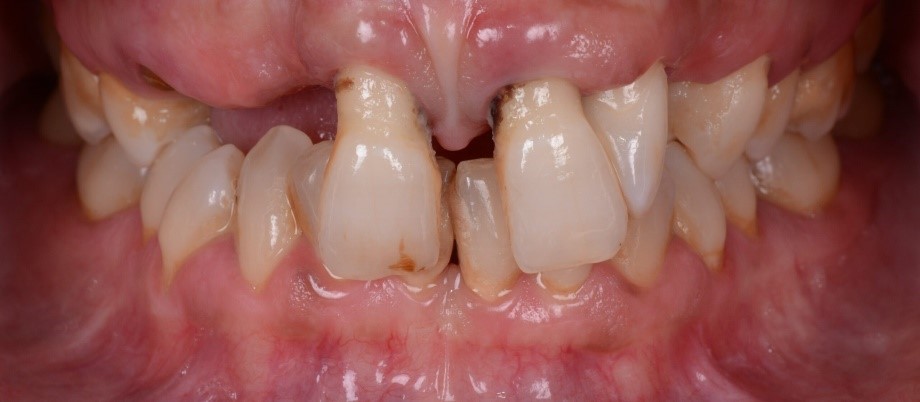
When this last stage occurs, there are no alternatives to implantology to restore correct and efficient masticatory functionality as well as the aesthetics of the smile.